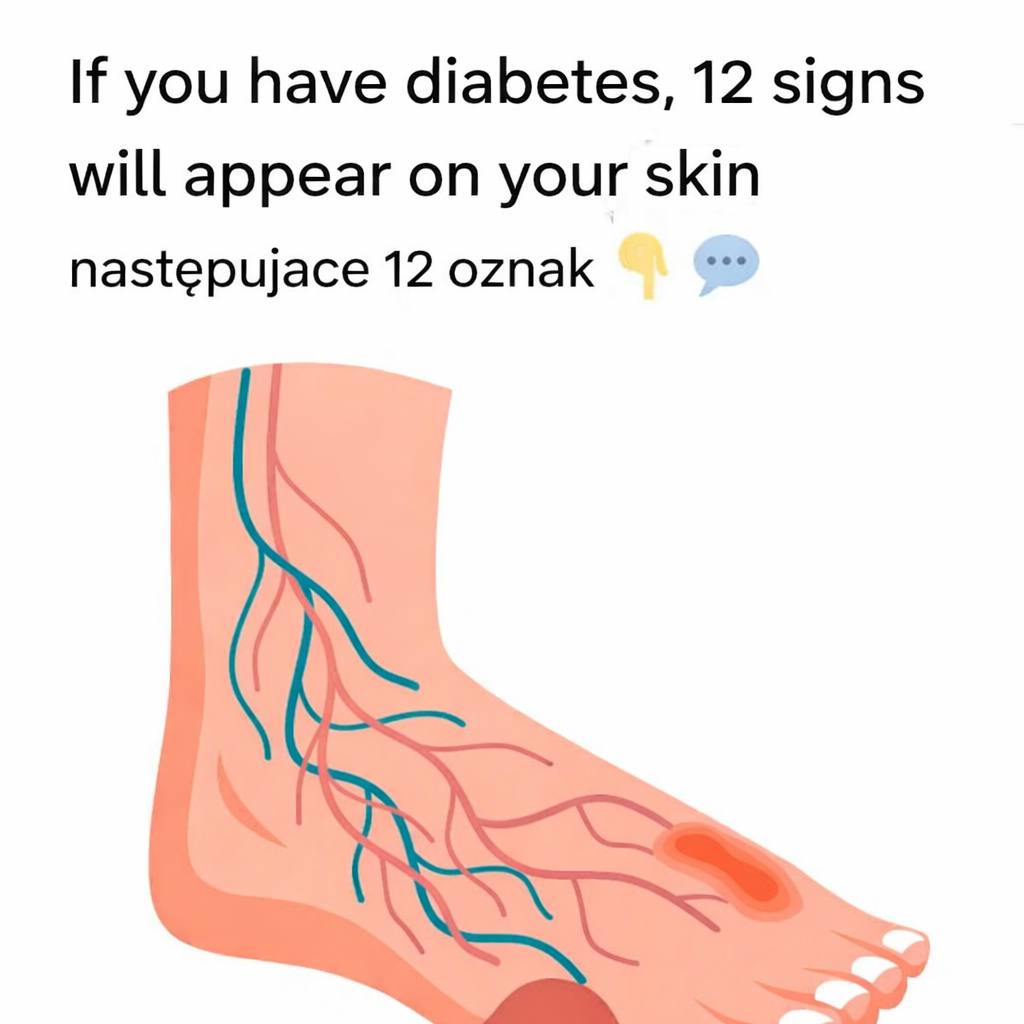
Have you ever noticed changes on your skin that surprised you? For people living with diabetes or who are at risk, the skin often acts as an early warning system, revealing clues about blood sugar levels and insulin effectiveness. It's important to take these diabetes-related skin problems seriously, as early detection can be crucial for effective treatment.
Surprisingly, in fact, one-third of people with diabetes will experience a related skin condition at some point. That's why we're highlighting 12 diabetes-related skin problems you shouldn't ignore.
From dark spots to wounds that won't heal, this guide breaks down each issue and decodes what it could mean for your overall well-being. Understand these key signs of diabetes on your skin, and you'll be better prepared to take action and seek appropriate care—potentially preventing larger health problems before they arise.
Diabetes-Related Skin Conditions
Diabetes can manifest itself in many ways, and the skin is no exception; it often serves as a window to hidden health problems. Many conditions, such as fat necrosis, which manifests as raised, shiny patches on the skin, or acanthosis nigricans, characterized by dark, velvety areas, usually around the neck folds and joints, are clear signs of high blood sugar and insulin resistance.
Some people may also experience digital callus – a condition in which the fingers become stiff – and diabetic blisters, which look remarkably similar to burn blisters, but without any prior trauma.
Skin infections remain a common problem in people with diabetes due to weakened immune systems; fungal infections, such as athlete's foot and athlete's foot, thrive in areas where moisture accumulates.
Diabetic dermopathy manifests itself through light brown, scaly patches that typically appear on the shins—commonly called shin splints. Another symptom is eruptive xanthomatosis, which manifests as yellowish nodules surrounded by red halos, especially when